Do you require any assistance? Simply reserve your appointment online below
Minimally Invasive Spine Surgery
Enhancing a quicker recovery
Minimally invasive spinal surgery (MISS) is an endoscopic procedure that uses specialized video cameras and instruments that are passed through small incisions (less than 2 cm) in the back, chest or abdomen to access the spine and perform the needed surgery.
Whenever possible, we at NSOC prefer to perform minimally invasive spine surgery rather than “open” procedures. Minimally invasive surgery uses smaller incisions, which minimizes the disruption to the spine and surrounding soft tissue, decreases muscle tearing and blood loss, reduces pain and risk, and speeds up recuperation.
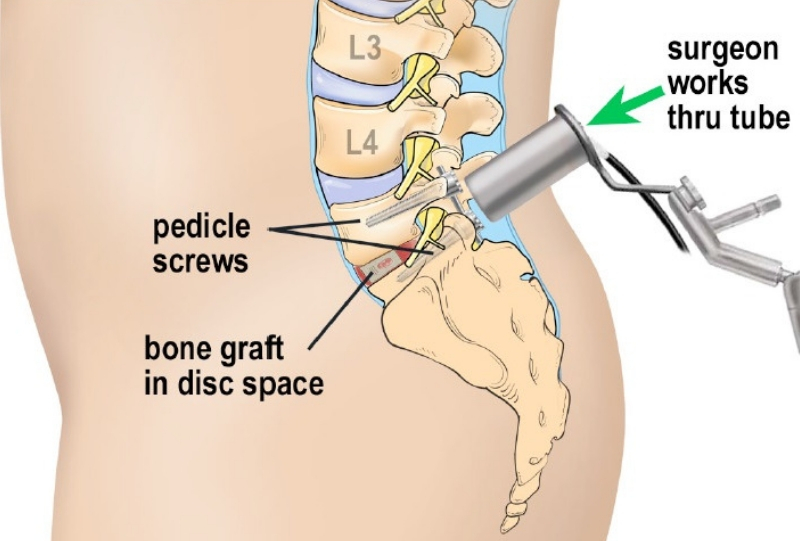
Why might you need a minimally invasive spinal surgery?

Most people who have back pain will not need surgery. Your healthcare provider might advise spine surgery if you have a back problem that hasn’t gotten better with another treatment, such as medicine or physical therapy. If you still have a lot of pain, surgery on your spine might fix the problem.
This treatment option is used to treat a variety of spine conditions such as:
Herniated disc
Spinal stenosis (narrowing of the spinal canal)
Spinal deformities (like scoliosis)
Spondylolysis (a defect in part of a lower vertebrae)
Common minimally invasive spine surgeries
NSOC offers a variety of minimally invasive spine surgeries including:
- Minimally invasive foraminotomy, laminectomy, and diskectomy enable us to treat nerve compression by making a small incision in your back and spreading the muscles away from the affected area. The nerve is freed from the compressing disc, bone, or ligaments.
- Minimally invasive fusion uses advanced imaging technology to guide the surgical instruments through a small, tube-shaped retractor.
- Vertebroplasty and kyphoplasty require small incisions. We expand your compressed bone using a type of bone cement that corrects bone height and deformity.
- Thoracoscopic thoracic surgery involves placing a to view the spine and affected nerves. It helps to remove the herniated disc with minimal disruption to spinal stability
What are the benefits of minimally invasive spine surgery?
Minimally invasive spine surgery offers several advantages over open surgery, which typically requires large incisions, muscle stripping, more anesthesia, a long hospital stay, and a long recuperation period. The benefits of spine surgery include:
- A few tiny scars instead of one large scar
- Shorter hospital stay – a few days instead of a week
- Reduced postoperative pain
- Shorter recovery time – a few months instead of a year – and quicker return to daily activities, including work
- Less blood loss during surgery
- Reduced risk of infection

Is Minimally Invasive Spinal Surgery Safe?

As with any surgical procedure, including minimally invasive spinal surgery, there are general risks and procedure-specific risks.
Most common general risks of spine surgery include the risk of adverse reactions to the anesthetic, post-operative pneumonia, blood clots in the legs (deep vein thrombosis) that may travel to the lungs (pulmonary embolus), infection at the site of surgery and blood loss during surgery therefore requiring a transfusion.
On rare occasions, during a minimally invasive procedure, the planned surgery cannot be completed and requires either a second trip to the operating room or a conversion from the minimally invasive technique to a full open technique.
It’s time to go back to doing what you love
What happens during a minimally invasive spinal surgery?
Most types of minimally invasive surgery rely on a thin telescope-like instrument, called an endoscope, or on a portable X-ray machine, called a fluoroscope, to guide the surgeon while he or she is working.
The endoscope is inserted through small incisions in the body. The endoscope is attached to a tiny video camera – smaller than a dime – which projects an internal view of the patient’s body onto television screens in the operating room.
Small surgical instruments are passed through one or more half-inch incisions, which are later closed with sutures and covered with surgical tape. The fluoroscope is positioned around the patient to give the surgeon the best X-ray views from which to see the anatomy of the spine.

Recovery after minimally invasive spinal surgery
The general healing time after minimally invasive spine surgery is less when compared to the standard open approach. This is due to the small incision and minimal disruption of the lumbar muscles during the minimally invasive spinal procedure.
Some procedures, such as radiofrequency surgery for spinal tumors or kyphoplasty to stabilize a vertebral compression fracture heal quite quickly and carry few post-operative restrictions. Other procedures performed in a minimally invasive fashion, such as a lumbar fusion surgery, heal more slowly based on the rate of bony fusing taking place in your spine.
To help you regain strength and speed your recovery, your doctor may recommend physical therapy. This will depend on the procedure and your general physical condition. Specific exercises will help you become strong enough to return to work and daily activities.
