Do you require any assistance? Simply reserve your appointment online below
Acromioclavicular Joint Sprain
We’ve got you Covered
Acromioclavicular joint sprain refers to an injury where the ligaments supporting the Acromioclavicular joint are overstretched.
The degree of Acromioclavicular joint sprain can vary from a mild strain of one or more of the surrounding ligaments to complete ligament tears and deformity.
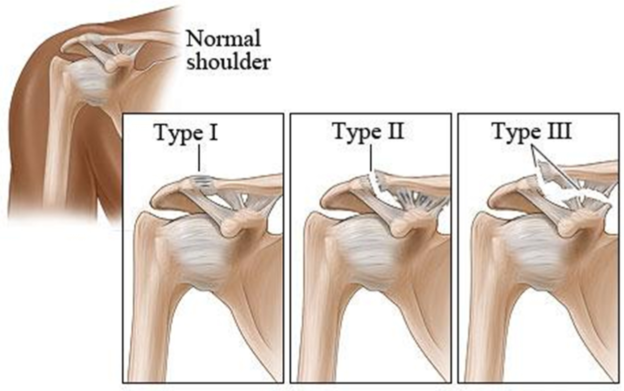
What is Acromioclavcular joint sprain
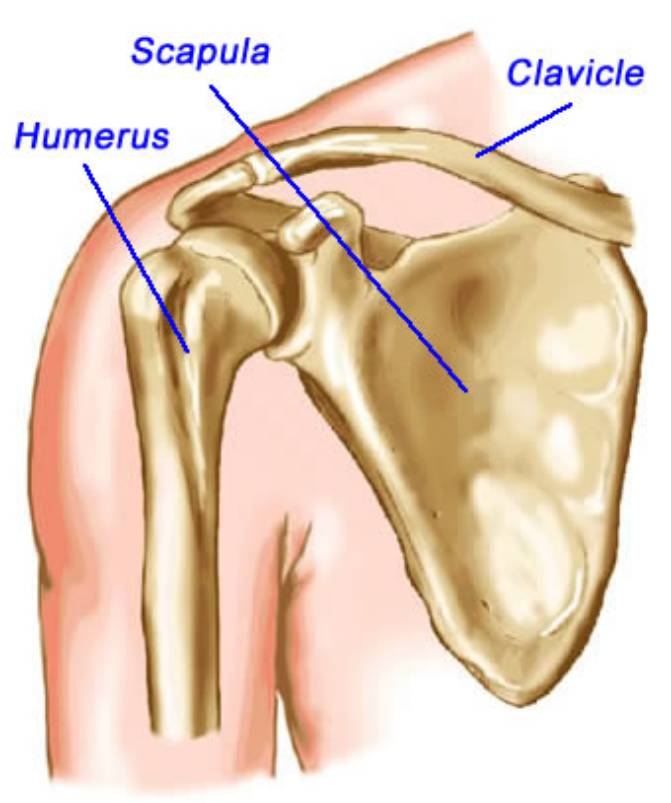
The shoulder joint is formed at the junction of three bones: the collarbone (clavicle), the shoulder blade (scapula), and the arm bone (humerus). The scapula and clavicle form the socket of the joint, and the humerus has a round head that fits within this socket. The end of the scapula is called the acromion, and the joint between this part of the scapula and clavicle is called the acromioclavicular joint.
When the acromioclavicular joint is disrupted, it is called a shoulder separation and can form a “step” if displaced. Another name for this injury is an acromioclavicular joint separation, or Acromioclavicular separation or an Acromioclavicular joint sprain.
The ligaments that hold the joints together are the acromioclavicular, coracoacromial and coracoclavicular (trapezoid and conoid) ligaments.
Causes of Acromioclavicular joint sprain
Direct forces can injure your Acromioclavicular joint when a person collides with a solid object or surface such as a fall from a bicycle or during a football tackle where the shoulder hits the ground.
when a person falls on an outstretched arm, the acromioclavicular joint sprain may also be injured indirectly
The contact force is transmitted up through the arm, which forces a separation of the acromion and clavicle.
The ligaments are overstretched and damaged in the process.
Signs and symptoms of Acromioclavicular joint sprain
- Pain on the top of the shoulder aggravated by heavy lifting, overhead and across body movements.
- Swelling +/- bruising.
- Loss of shoulder movement.
- Sometimes a hard, visible lump may also be present on the top of the shoulder, indicating displacement of the clavicle (collar bone).
Acromioclavicular joint sprain injury is graded by severity from Grade I (minimal joint disruption) to Grade III (severe injury). If the injury is the more severe, Grade III, a bump caused by the separated AC joint may be seen or felt at the tip of the shoulder bones. The diagnosis of shoulder separation is often quite apparent from hearing a story that is typical of this injury, and a simple physical examination.
X-rays should be performed to ensure there is no fracture of these bones. Clavicle fractures from falls are particularly common.

Treatment of Acromioclavicular joint sprain
Physiotherapy
Most patients with Acromioclavicular joint sprain start to feel better within a few days or a week of the injury. However, full ligament healing will take at least six weeks. During this time it is important to protect your AC joint ligaments from overstretching the immature scar tissue. It can be helpful to use a sling, taping or a shoulder brace.
Surgical
In severe cases, some patients choose to undergo Acromioclavicular joint sprain surgery to pin the Acromioclavicular joint or repair the damaged ligaments surrounding the AC joint.
Your physiotherapist’s treatment will aim to:
- Reduce pain and inflammation.
- Normalize joint range of motion.
- Strengthen your shoulder.
- Improve your shoulder blade and shoulder alignment.
- Normalize your muscle lengths.
- Improve your upper limb proprioception.
- Improve your technique and function eg lifting, overhead activities.
- Minimize your chance of re-injury as you return to sport or work.

You are in Great Hands
Rehabilitation after Acromioclavicular joint sprain surgery
Post-operative rehabilitation is one of the most important, yet too often neglected, aspects of surgery. The quickest and most successful outcomes result from the guidance and supervision of an experienced shoulder physiotherapist.
Your rehabilitation following shoulder surgery of Acromioclavicular-joint sprain focuses on restoring full shoulder motion, strength, power and endurance. You will also require proprioception and functional-based retraining that is individualised towards your specific needs.
Risks of surgery include infection, persistent instability and pain, stiffness, and difficulty returning to your previous level of activity.

Removing the damaged femoral head and replacing it with a metal stem that is placed in the femur’s hollow center; the stem may be cemented or “press fitted” into the bone.
Placing a metal or ceramic ball on the upper part of the stem to replace the damaged femoral head.
Removing the damaged cartilage surface of the socket and replacing it with a metal socket; screws or cement may be used to hold the socket in place.
Inserting a plastic, ceramic or metal spacer between the new ball and the socket to create a smooth gliding surface.
